Call Us For Easy
Confidential Assistance
503-506-0101
It only takes 5 minutes to get started
Navigating Heroin and Opiate Withdrawal: Safe Inpatient Detox Options Near Eugene
Posted on: April 11th, 2026 by writer

Table of Contents
- What Actually Happens During Opioid Withdrawal?
- Oregon’s Opioid Emergency: What Eugene Residents Need to Know
- Cold Turkey vs. Medical Support: Why Inpatient Detox Has an 80% Success Rate
- Making Withdrawal Manageable: The Medications That Ease the Pain
- From Failed Outpatient Attempt to Successful Recovery: Why Medical Oversight Matters
- Choosing the Right Inpatient Detox Facility: A Checklist for Eugene Residents
- Final Thoughts
For many people trapped in the cycle of opioid addiction, there’s a paralyzing fear that overshadows every thought of recovery: the terror of withdrawal. On the streets, it’s known as “dope sickness”—a brutal constellation of physical and psychological symptoms so severe that facing another day seems impossible without the drug. This fear isn’t irrational; it’s a biological reality that keeps thousands of Oregonians locked in addiction, even when they desperately want to break free. Oregon is facing an unprecedented opioid crisis. Between 2019 and 2023, the state experienced a staggering 600% surge in opioid overdose deaths, with fentanyl now present in 77.7% of fatal cases. Here in Lane County, where Eugene residents live and work, opioid-related emergencies occur at significantly higher rates than the national average. The contaminated drug supply has transformed what was once a predictable (though painful) withdrawal process into a dangerous medical emergency requiring professional intervention. But here’s the critical message that could save your life or the life of someone you love: withdrawal doesn’t have to be faced alone, and it doesn’t have to be endured in agony. Medically supervised inpatient detox transforms an unbearable ordeal into a safe, manageable medical process. The statistics tell a hopeful story—over 80% of people who complete inpatient medical detox successfully transition to long-term treatment, compared to only 30-40% who attempt outpatient alternatives. Despite these encouraging numbers, less than 20% of individuals with opioid use disorder receive specialized treatment, with fear of withdrawal cited as the primary deterrent. This article will demystify what happens during opioid withdrawal, explain why inpatient medical detox is the gold standard for safety and success, and show Eugene residents how to access compassionate care that addresses both the physical pain and psychological barriers standing between addiction and recovery.
What Actually Happens During Opioid Withdrawal?
Understanding the withdrawal process begins with understanding what opioids do to your brain. When you use heroin, fentanyl, or prescription opioids regularly, these substances hijack specific receptors in your brain called mu-opioid receptors. These receptors naturally regulate pain, reward systems, and critical autonomic functions like breathing and heart rate. Over time, your brain adapts to the constant presence of opioids, reducing its own production of natural pain-relieving chemicals and pleasure-inducing neurotransmitters. This neurochemical dependence creates a biological trap. When opioid use stops—even for just a few hours—the sudden absence of receptor stimulation triggers a massive cascade of noradrenaline release. This chemical flood is what causes the characteristic symptoms of withdrawal: your nervous system, which had adapted to constant suppression, suddenly goes into overdrive.
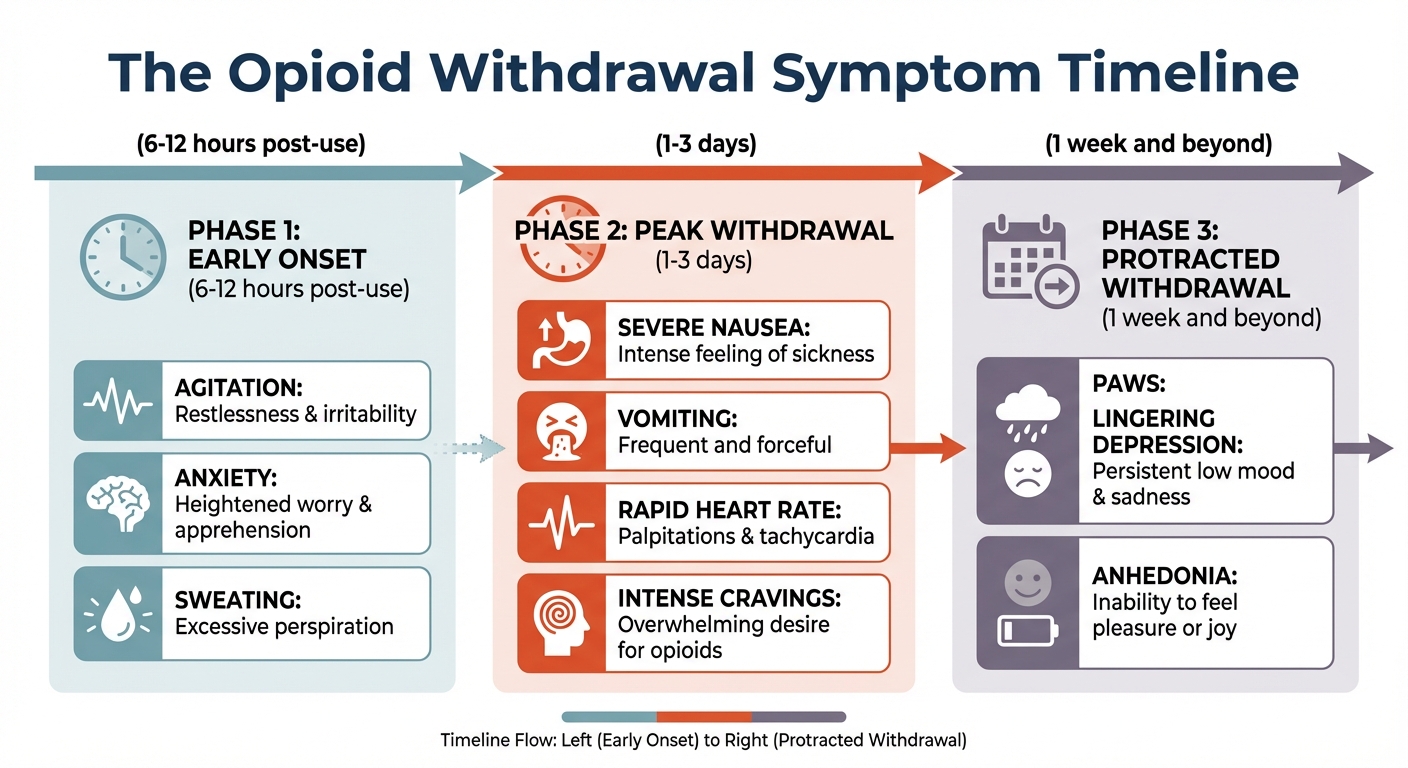
The progression of symptoms follows a predictable but brutal timeline. Within 6-12 hours of your last dose, early symptoms begin: anxiety that feels like impending doom, muscle aches that worsen with every movement, insomnia despite exhaustion, profuse sweating, and an agitation that makes sitting still impossible. These are just the opening act. Days 1-3 bring peak withdrawal, when symptoms reach their maximum intensity. Severe nausea transforms into violent vomiting that can lead to dangerous dehydration. Diarrhea and abdominal cramping occur simultaneously, causing further fluid loss. Your heart races, blood pressure spikes, and cravings become so overwhelming that every fiber of your being screams for relief. During this phase, the path of least resistance—relapse—becomes almost irresistible without medical support.
Important to Know
Even after the acute physical symptoms subside around day 7, many people experience Post-Acute Withdrawal Syndrome (PAWS)—a constellation of psychological symptoms including depression, anxiety, and anhedonia (the inability to feel pleasure) that can persist for months. This protracted phase catches many people off guard, leading to relapse weeks or even months into recovery when they mistakenly believe the worst is behind them.
The modern opioid crisis has added another dangerous variable: fentanyl. Today’s street heroin is frequently contaminated with this synthetic opioid, which is 50-100 times more potent than morphine. Fentanyl’s unique properties—particularly its tendency to store in fat tissue and release slowly over time—make withdrawal even more unpredictable and dangerous. This complication has rendered traditional “cold turkey” approaches not just ineffective but potentially life-threatening.
Oregon’s Opioid Emergency: What Eugene Residents Need to Know
The numbers paint a sobering picture of the crisis unfolding in our communities. Oregon’s 600% increase in opioid overdose deaths from 2019 to 2023 isn’t just a statistic—it represents hundreds of families shattered by loss, countless individuals trapped in addiction, and a healthcare system struggling to respond to an unprecedented emergency.
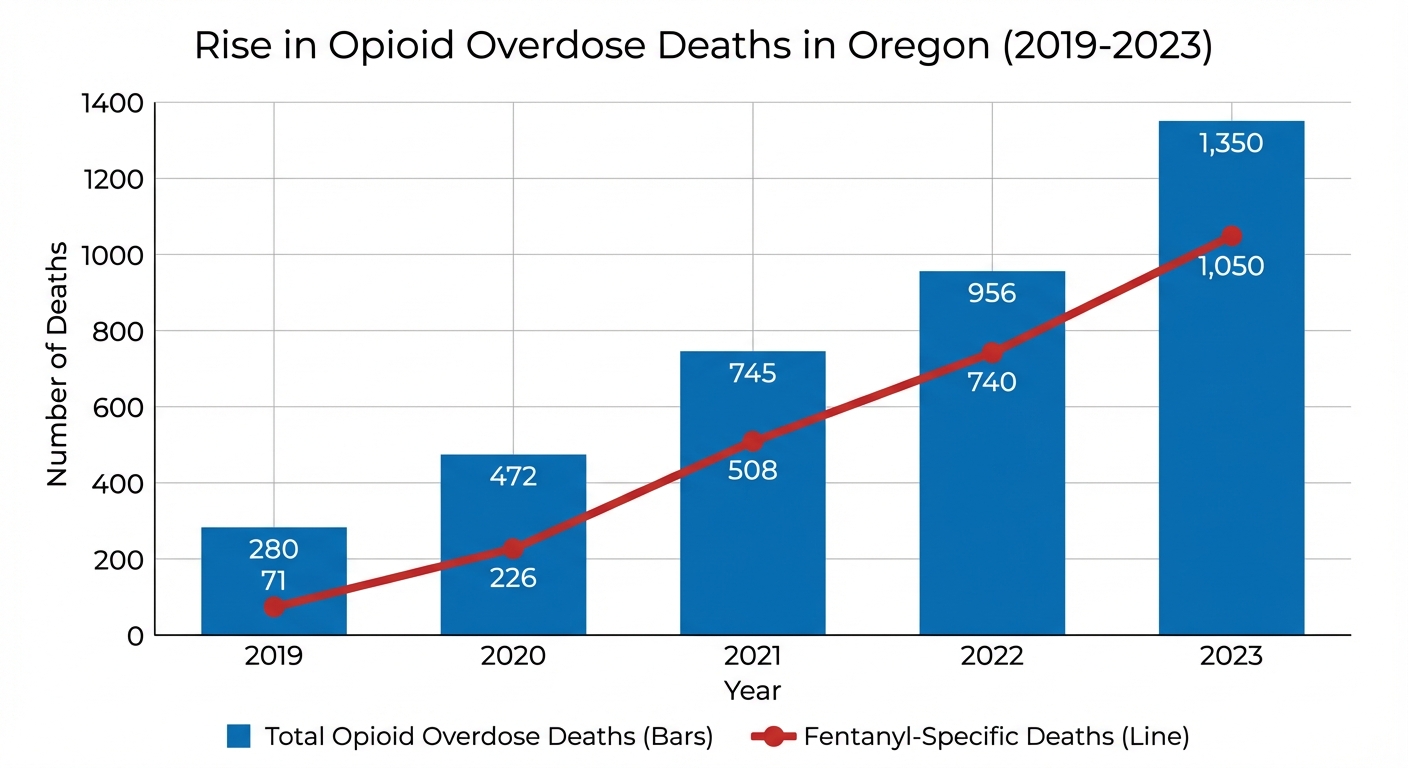
The data reveals an alarming acceleration. In 2019, Oregon recorded 280 total opioid overdose deaths, with fentanyl involved in just 25.3% of cases. By 2023, that number had exploded to 1,350 deaths, with fentanyl present in over 77% of fatalities. This dramatic shift reflects the contamination of the drug supply—people who think they’re using heroin are unknowingly consuming lethal doses of fentanyl.
Lane County’s Specific Challenges
Lane County faces specific challenges that make local access to medical detox even more critical:
- The region has historically experienced higher-than-average opioid prescribing rates, creating a pipeline of individuals who transition from prescription painkillers to illicit substances
- Emergency departments in Eugene report significantly elevated rates of visits related to illicit drug use compared to national benchmarks, indicating widespread untreated addiction in the community
- A massive treatment gap persists: less than 20% of people with opioid use disorder receive specialized treatment
This gap exists for multiple reasons, but two barriers stand out: the paralyzing fear of withdrawal and the lack of accessible medical detox services. Many people cycle through repeated attempts to quit on their own, suffering through days of agony before relapsing—sometimes fatally—because they didn’t know that professional medical support could make the process manageable.
Geographic Considerations
Facilities located near but outside Eugene—like Pacific Ridge—offer a critical strategic advantage. They remove individuals from local drug networks and environmental triggers (the street corners, familiar faces, and old haunts that pull people back into use) while remaining accessible enough for families to stay connected during treatment. This balance between distance and accessibility can make the difference between successful recovery and another failed attempt.
With fentanyl now dominating Oregon’s illicit opioid supply, attempting detox without medical oversight dramatically increases overdose risk upon relapse. When someone relapses after a period of abstinence, their tolerance has decreased significantly, making the same dose they used before potentially fatal. Professional medical detox doesn’t just ease suffering—it establishes a medically supervised bridge to ongoing treatment that dramatically reduces the risk of deadly relapse.
Cold Turkey vs. Medical Support: Why Inpatient Detox Has an 80% Success Rate
For decades, the prevailing approach to opioid detox was “social detox”—essentially stopping drug use abruptly (going “cold turkey”) in a supervised but non-medical environment. The philosophy was grimly simple: tough it out, endure the suffering, and emerge on the other side. Today, the American Society of Addiction Medicine strongly discourages this approach for opioid dependence, citing unnecessary patient suffering, high dropout rates, and elevated risk of fatal overdose upon relapse. The evidence base has definitively shifted toward medical intervention. Modern addiction medicine recognizes opioid withdrawal as a medical condition requiring professional treatment, not a moral failing requiring punishment.
The Outpatient Challenge
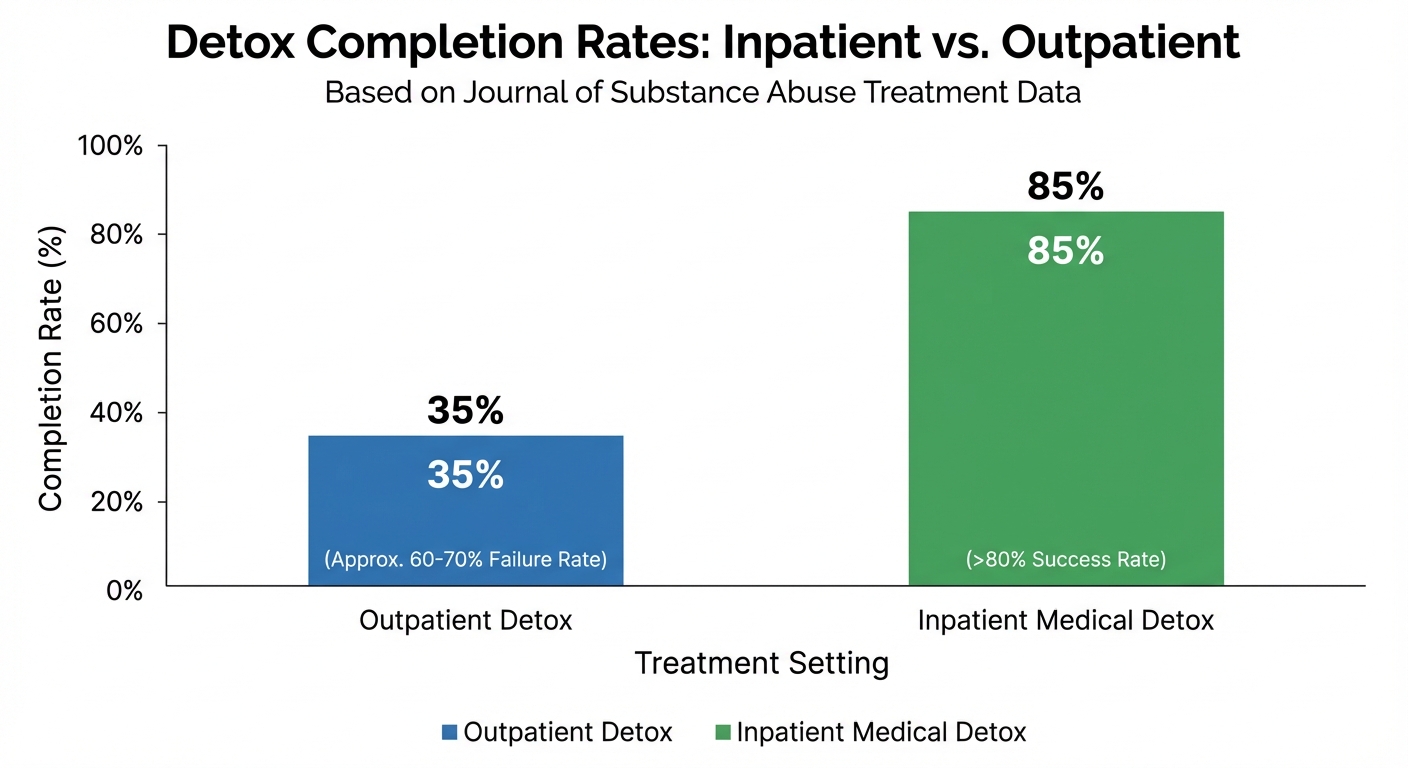
Outpatient detox represents a middle ground—patients receive medications to manage symptoms but remain in their home environment. While theoretically sound, outpatient approaches face significant practical challenges. Studies show that 60-70% of patients fail to complete outpatient detox programs. The reasons are predictable:
- Constant exposure to environmental triggers
- Immediate access to drugs when symptoms become unbearable
- Lack of around-the-clock medical monitoring
- Inadequate support for the intense psychological components of withdrawal
For severe cases—particularly those complicated by fentanyl—outpatient care is simply inadequate. The medication timing required to avoid precipitated withdrawal demands clinical expertise and constant monitoring that home-based treatment cannot provide.
The Inpatient Advantage
Inpatient medical detox offers comprehensive advantages that explain its dramatically higher success rate:
| Benefit | Why It Matters |
|---|---|
| 24/7 Medical Supervision | Vital signs continuously monitored; immediate response to complications |
| Geographic Separation | Removal from drug networks and environmental triggers |
| Comprehensive Medication Management | Addresses physical symptoms and underlying neurochemical imbalances |
| Psychological Support | Trained specialists provide emotional support during vulnerable phases |
| Structured Environment | Therapeutic container strong enough to hold patients through the storm |
Perhaps most importantly, inpatient care provides psychological support during the most vulnerable phase of recovery. Trained addiction specialists understand the emotional rollercoaster of detox—the despair, the bargaining, the moments of clarity followed by intense cravings. This human element, combined with medical expertise, creates a container strong enough to hold someone through the storm.
“Over 80% of patients who enter inpatient medical detox complete the program successfully and transition to long-term treatment. Research published in the Journal of Substance Abuse Treatment confirms that inpatient detox serves as an effective bridge to sustained recovery, with completion and transition-to-treatment rates far exceeding alternative approaches.”
Making Withdrawal Manageable: The Medications That Ease the Pain
Modern medical detox represents a fundamental shift in treatment philosophy. The goal isn’t to punish people for their addiction or force them to “tough it out”—it’s to ease suffering while safely stabilizing their neurochemistry. Evidence-based pharmacological interventions can transform withdrawal from an unbearable ordeal into a manageable medical process.
FDA-Approved Medications for Opioid Use Disorder (MOUD)
The cornerstone of modern treatment involves medications specifically designed to address opioid dependence: Buprenorphine is a partial opioid agonist that binds to the same brain receptors as heroin but doesn’t produce euphoria. It eliminates cravings and withdrawal symptoms while blocking the effects of other opioids, creating a stable platform for recovery. The key advantage: when administered correctly, it prevents precipitated withdrawal while allowing the brain to gradually readjust. Methadone, a full opioid agonist, is used in controlled clinical settings to safely taper patients off potent opioids. While it activates the same receptors as heroin, it does so in a controlled, predictable manner that stabilizes patients without producing a high. Methadone’s long half-life means once-daily dosing provides steady symptom relief.
Supporting Medications
Beyond opioid replacement, clinicians use additional medications to target specific withdrawal symptoms:
- Alpha-2 Adrenergic Agonists (clonidine, lofexidine) suppress the autonomic nervous system hyperactivity that causes sweating, rapid heart rate, muscle cramps, and anxiety
- Antiemetics (ondansetron) combat severe nausea and vomiting
- Antispasmodics ease muscle cramps and gastrointestinal cramping
- Non-narcotic sleep aids address the profound insomnia that makes early recovery feel impossible
- IV fluids prevent dangerous dehydration when patients can’t keep food or liquids down
Individualized Treatment Protocols
What makes modern medical detox truly effective is individualization. Treatment protocols are tailored to each patient’s specific situation—the particular opioid they’ve been using, their duration and intensity of use, any co-occurring medical conditions, and their previous treatment history. This personalized approach is especially critical for patients using fentanyl-contaminated heroin, who require specialized “micro-dosing” protocols for safe buprenorphine induction.
The medical supervision ensures medications are administered at precisely the right times to maximize comfort while avoiding complications. Clinicians monitor patients’ responses and adjust protocols in real-time, something impossible in outpatient settings where patients self-administer medications at home.
From Failed Outpatient Attempt to Successful Recovery: Why Medical Oversight Matters
The difference between outpatient and inpatient approaches becomes starkly clear in real-world cases, particularly with modern fentanyl-complicated addiction. Consider a 32-year-old man with a five-year history of IV heroin use who unknowingly began consuming fentanyl-contaminated drugs—a scenario playing out across Eugene and Oregon every day.
The Failed Outpatient Attempt
His first attempt at recovery involved outpatient buprenorphine detox. The plan seemed straightforward: wait until experiencing moderate withdrawal symptoms, then take the first dose of buprenorphine. However, fentanyl’s unique pharmacology created a dangerous trap. Unlike heroin, which clears the system relatively quickly, fentanyl is lipophilic—it stores in fat tissue and releases slowly over days. This means someone can feel like they’re in withdrawal while still having significant opioid activity in their system. When this patient took buprenorphine too early, it triggered precipitated withdrawal—a sudden, violent onset of severe symptoms far worse than natural withdrawal. Buprenorphine, with its higher receptor affinity, essentially ripped fentanyl off his brain receptors, causing an immediate, agonizing crash. The experience was so traumatic that he relapsed within 24 hours, using a large dose to compensate—exactly the scenario that leads to fatal overdoses.
The Successful Inpatient Experience
Recognizing the danger, he was admitted to an inpatient medical detox facility. The clinical team employed the Bernese method—a specialized micro-dosing protocol for buprenorphine induction in fentanyl users. Instead of waiting for full withdrawal and taking a standard dose, they started with tiny amounts of buprenorphine while he was still using, gradually building up the dose over several days under constant medical monitoring.
What Made the Difference
Throughout the seven-day process, he received:
- IV fluids to prevent dehydration
- Clonidine to manage autonomic symptoms
- Around-the-clock nursing care
- Immediate support when cravings became overwhelming at 2 AM
- Medical intervention when blood pressure spiked dangerously
- Professional counseling to work through emotional turbulence
He completed the detox with minimal discomfort and successfully transitioned to a 30-day residential rehabilitation program. The difference wasn’t willpower or motivation—he had those during his failed outpatient attempt. The difference was the nuanced clinical oversight that only inpatient facilities can provide. This case illustrates why Eugene residents facing today’s contaminated drug supply need professional medical supervision. The opioids on the street aren’t the same drugs people were using five years ago. Fentanyl has changed the game, requiring specialized knowledge and round-the-clock monitoring that home-based treatment simply cannot offer.
Choosing the Right Inpatient Detox Facility: A Checklist for Eugene Residents
Not all detox programs are created equal. When your life—or your loved one’s life—depends on successful treatment, understanding what to look for in a quality facility becomes critically important.
Essential Criteria for Quality Care
| Criteria | What to Look For |
|---|---|
| Medical Staffing | 24/7 coverage with physicians, RNs, and addiction specialists on-site at all times |
| Evidence-Based MOUD | Buprenorphine, methadone access, comfort medications, fentanyl protocols |
| Individualized Plans | Comprehensive assessments, customized protocols, real-time adjustments |
| Environment | Comfortable, secure, removed from triggers, therapeutic atmosphere |
| Continuing Care | Clear pathways to residential rehab or intensive outpatient programs |
| Financial Access | Insurance acceptance, state/federal program options, transparent pricing |
| Family Involvement | Education components, communication updates, loved one support |
Questions to Ask Before Admission
When evaluating facilities, don’t hesitate to ask direct questions:
- What’s your completion rate?
- What percentage of patients successfully transition to continued treatment?
- How do you handle medical emergencies?
- What’s your staff-to-patient ratio?
- Are your clinicians specifically trained in addiction medicine?
- What specialized protocols do you use for fentanyl-complicated cases?
- How do you coordinate with continuing care providers?
For Eugene Residents
Facilities like Pacific Ridge offer the combination of professional medical expertise, comfortable environments, and strategic geographic placement that creates optimal conditions for successful detox and transition to long-term recovery. Located close enough to maintain family connections but far enough to provide separation from local triggers, these facilities represent the balance many Eugene residents need for successful treatment.
Final Thoughts
The fear of withdrawal is real, valid, and deeply rooted in biological reality. For too long, that fear has acted as an insurmountable barrier, keeping people trapped in addiction despite their desperate desire for freedom. But the landscape of addiction treatment has transformed dramatically—withdrawal no longer has to be a death sentence or an agonizing ordeal endured alone. Modern medical detox has revolutionized the first critical step of recovery. What was once considered an unavoidable crucible of suffering has become a manageable medical process, guided by evidence-based protocols and compassionate professionals who understand exactly what you’re experiencing. The transformation from “dope sickness” to medically supported stabilization can literally save your life. For Eugene residents facing opioid addiction, the urgency of accessing professional care has never been greater. With fentanyl present in over 77% of Oregon’s fatal overdoses, the contaminated drug supply has made attempting detox without medical supervision not just difficult but potentially deadly. The same dose that provided relief yesterday could be fatal tomorrow. The same withdrawal process that was merely excruciating five years ago now carries life-threatening complications that require expert medical management.
“The statistics offer genuine hope: over 80% of people who complete inpatient medical detox successfully transition to long-term treatment. This isn’t just about getting through the immediate crisis—it’s about establishing a stable foundation for sustained recovery.”
Recovery is possible. The first step is recognizing that help is available and that suffering through withdrawal alone is unnecessary. You don’t have to be strong enough to endure “dope sickness”—you just have to be brave enough to reach out for professional support.
Ready to Take the First Step?
If you or someone you love is struggling with opioid addiction in the Eugene area, Pacific Ridge offers comprehensive, medically supervised inpatient detox services designed specifically for the challenges of modern opioid withdrawal. Our evidence-based protocols, experienced medical staff, and compassionate approach transform the fear of withdrawal into a manageable journey toward recovery.
Don’t let another day be stolen by addiction.
For immediate, free, confidential support 24 hours a day, call SAMHSA’s National Helpline at 1-800-662-4357.
The path to freedom begins with a single step. Let us help you take it safely.
References
- Oregon Health Authority. (2024). Oregon Opioid Data Dashboard. https://www.oregon.gov/oha/ph/preventionwellness/substanceuse/opioids/pages/data.aspx
- Substance Abuse and Mental Health Services Administration (SAMHSA). (2023). National Survey on Drug Use and Health (NSDUH). https://www.samhsa.gov/data/data-we-collect/nsduh-national-survey-drug-use-and-health
- National Center for Biotechnology Information (NCBI). (2022). Clinical Management of Opioid Withdrawal. https://www.ncbi.nlm.nih.gov/books/NBK310652/
- National Institute on Drug Abuse (NIDA). (2021). Heroin Research Report: What are the treatments for heroin use disorder? https://nida.nih.gov/publications/research-reports/heroin/what-are-treatments-heroin-use-disorder
- American Society of Addiction Medicine (ASAM). (2020). The ASAM National Practice Guideline for the Treatment of Opioid Use Disorder. https://www.asam.org/quality-care/clinical-guidelines/national-practice-guideline
- Day, E., & Strang, J. (2011). Outpatient versus Inpatient Opioid Detoxification: A Randomized Controlled Trial. Journal of Substance Abuse Treatment. https://pubmed.ncbi.nlm.nih.gov/21036514/
- Substance Abuse and Mental Health Services Administration (SAMHSA). (2015). TIP 45: Detoxification and Substance Abuse Treatment. https://store.samhsa.gov/sites/default/files/d7/priv/sma15-4131.pdf
- National Library of Medicine (NIH). (2021). Microdosing Buprenorphine Induction for the Treatment of Opioid Use Disorder. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8213340/
Posted in Treatment
Recent Posts
- Navigating Heroin and Opiate Withdrawal: Safe Inpatient Detox Options Near Eugene
- Confidential Cocaine Addiction Treatment: A Guide for Portland Professionals
- Dual Diagnosis Rehab Near Salem: Treating Alcoholism and Depression Together
- Meth Addiction Treatment for Eugene Residents: The Willamette Valley Healing Advantage
Are you looking for help?
Pacific Ridge is a residential drug and alcohol treatment facility about an hour from Portland, Oregon, on the outskirts of Salem. We’re here to help individuals and families begin the road to recovery from addiction. Our clients receive quality care without paying the high price of a hospital. Most of our clients come from Oregon and Washington, with many coming from other states as well.
Pacific Ridge is a private alcohol and drug rehab. To be a part of our treatment program, the client must voluntarily agree to cooperate with treatment. Most intakes can be scheduled within 24-48 hours.
Pacific Ridge is a State-licensed detox and residential treatment program for both alcohol and drugs. We provide individualized treatment options, work closely with managed care organizations, and maintain contracts with most insurance companies.

Quick links
Recent Posts
- Navigating Heroin and Opiate Withdrawal: Safe Inpatient Detox Options Near Eugene
- Confidential Cocaine Addiction Treatment: A Guide for Portland Professionals
- Dual Diagnosis Rehab Near Salem: Treating Alcoholism and Depression Together
- Meth Addiction Treatment for Eugene Residents: The Willamette Valley Healing Advantage
Contact Us
Pacific Ridge- 1587 Pacific Ridge Ln SE
Jefferson, OR 97352 - Email:
[email protected] - Phone:
503-506-0101 - Fax:
503-581-8292
- Copyright © 2026 Pacific Ridge - All Rights Reserved. Web Design & SEO by Lithium
- Follow us on

